Achieving Better Health Outcomes Through Advanced Bio-Monitoring Wearables
Biosensors are analytical devices that convert a biological response into an electrical signal. The biosensors must be highly specific, independent of physical parameters such as pH and temperature and should be reusable. These devices help healthcare practitioners screen for, diagnose, and treat multiple medical conditions in the home and clinical environments. From simple pregnancy tests to smart wearable technology, biosensors offer non-invasive methods to detect the presence of chemicals and compounds that might indicate illness. Based on the bioreceptor, biosensors are classified as enzymatic biosensors (most common class), immunosensors (possess high specificity and sensitivity and are specifically useful in diagnosis), aptamer or nucleic acid-based biosensors (possess high specificity for microbial strains and nucleic acid.
Wearable technology in healthcare refers to devices that patients attach to their bodies to collect health and fitness data, which they may provide to doctors, health providers, insurers and other relevant parties. Examples include fitness trackers, blood pressure monitors and biosensors. Wearable biosensors are devices that can be worn on, inside, or near the human body to monitor biological signals, such as indicators of a patient's health. They provide continuous measurements of dynamic physiological parameters in real time, providing a digital output that can easily be interpreted and acted upon. The future of wearable technology in healthcare is promising, with emerging trends such as smart clothing, advanced sensors, and augmented reality. These technologies have the potential to revolutionize healthcare by enabling more accurate and personalized diagnosis and treatment of medical conditions. Modern wearable technology falls under a broad spectrum of usability, including smartwatches, fitness trackers such as the Fitbit Charge, VR headsets, smart jewelry, web-enabled glasses and Bluetooth headsets. Artificial intelligence and wearable technology can now be used to assess and provide feedback on the ergonomic risks posed by high impact and repetitive tasks, making it quicker and easier to identify ways of improving training and work processes to reduce the risk of musculoskeletal injuries. As these devices track and monitor personal health data, such as heart rate, activity levels, and sleep patterns, they collect a significant amount of personal data. This data is often stored in the cloud, and third-party access is granted to companies and researchers who may use this data for various purposes.[1]
Common use cases for medical-grade wearables include monitoring patients at home after surgery or assisting patients with self-management of diabetes, hypertension or other chronic conditions. The other category is consumer-grade wearables, which include watches, rings and articles of clothing. The most common uses for wearable technology are for helping to monitor and alert the wearer about their personal health information or for social communication purposes – like calling, texting, social media, etc These sensors monitor vital signs in various individuals, including patients, athletes, infants, and the elderly. They contribute to mobile health technologies, offering real-time health recommendations and management. Wearable and implantable devices are reshaping healthcare, driven by sensor advancements. Wearable devices are soon expected to forecast changes in health, mood, and stress as well as measure blood alcohol content, athletic performance, heart condition, and age-related diseases.[2]
Photo by FitNish Media on Unsplash
Key Market Insights
The wearable medical devices market size was valued at USD 59.12 billion in 2022 and is projected to grow from USD 73.77 billion in 2023 to USD 428.92 billion by 2030, exhibiting a GR of 28.6% during 2023-2030. North America dominated the global market with a share of 33.69% in 2022.[3]
Working Of Wearable Devices
Wearable tech healthcare brings 4 main functions that are currently used to serve in healthcare. including: monitoring, screening, detection, and prediction
· Monitoring: Monitoring is the basic function served by wearables, performed by wristbands, patches, watches and clothing. It involves the continuous collection of data from individuals or specific populations. Wearables are particularly efficient for monitoring as they can track various biomedical processes using different sensors and can be worn constantly for continuous data collection.
· Screening: Screening involves identifying specific conditions or individuals associated with those conditions within the datasets collected through monitoring. Wearables used for screening often utilize passive sensors that measure motion, steps, light, pressure, sound, and other factors. For example, wearable garments have been used to monitor individuals during sleep and screen for sleep apnea.
· Detection: When wearables monitor specific conditions in populations, they can be used to detect and alert individuals about those conditions. Detection involves analyzing wearable data collected through monitoring to identify patterns and features that can be interpreted as indicators of specific biomedical conditions. For instance, smartwatches and dedicated bands have been used for heart rate monitoring and automatic detection of atrial fibrillation. Detection also intersects with both monitoring and screening. For example, smartwatches can monitor populations for irregular pulse, screen for individuals potentially suffering from atrial fibrillation, and identify the condition.
· Prediction: Prediction involves inferring future trends or events of interest for the biomedical study of populations based on monitoring data. Currently, only a few wearable devices are used for prediction in the health context. They can be used to predict outcomes such as mortality, readmissions, and clinical risk. In the context of COVID-19, wearables have been tested for retrospective detection of infection and prediction of COVID-19, even before the presence of symptoms. Other examples include using accelerometer data from wearable devices to predict biological age and mortality and respiratory rate data to predict exacerbations of chronic obstructive pulmonary disease.
Biomonitoring And Wearables – A Great Help In Achieving Health Outcomes
Health monitoring wearable devices perform following actions:
· Collect data and share with healthcare professionals: Wearable tech in health is equipped with microprocessors, batteries, and internet connectivity, allowing the collected data to be synchronized with other electronic devices like smartphones or laptops. This data then will be shared and forwarded directly to patient management center for healthcare professionals.
· Built-in sensors and tracking capabilities: Wearables are equipped with built-in sensors that enable various functionalities, such as tracking bodily movements, providing biometric identification, or assisting with location tracking. For instance, activity trackers and smartwatches, which are among the most popular types of wearables, are worn on the wrist and continuously monitor physical activities and vital signs throughout the day.
· Different forms and tracking methods: While many wearables are designed to be worn on the body or attached to clothing, some function without physical contact with the user. Devices like cell phones, smart tags, or computers can be carried around to track user movements. Others rely on remote smart sensors and accelerometers to monitor movements and speed, while some utilize optical sensors for measuring heart rate or glucose levels. Regardless of the specific technology, all these wearables share the common feature of real-time data monitoring.
Benefits Of Biosensors/Wearable Devices In Healthcare
Photo by Alora Griffiths on Unsplash
Despite the progress to date in the development of wearable sensors, there are still several limitations in the accuracy of the data collected, precise disease diagnosis, and early treatment. This necessitates advances in applied materials and structures and using artificial intelligence (AI)-enabled wearable sensors to extract target signals for accurate clinical decision making and efficient medical care. Artificial intelligence (AI)-based wearable sensors can collect, analyze, and transmit real-time health data to healthcare providers so that they can make efficient decisions based on patient data. Therefore, wearable sensors have become increasingly popular due to their ability to provide a non-invasive and convenient means of monitoring patient health. These wearable sensors can track various health parameters, such as heart rate, blood pressure, oxygen saturation, skin temperature, physical activity levels, sleep patterns, and biochemical markers, such as glucose, cortisol, lactates, electrolytes, pH and environmental parameters.
Wearable health technology includes first-generation wearable technologies, such as fitness trackers, smartwatches, and current wearable sensors, and is a powerful tool in addressing healthcare challenges. The data collected by wearable sensors can be analyzed using machine learning (ML) and AI algorithms to provide insights into an individual’s health status, enabling early detection of health issues and the provision of personalized healthcare. One of the most significant advantages of AI-based wearable health technology is to promote preventive healthcare. This enables individuals and healthcare providers to proactively address symptomatic conditions before they become more severe. Wearable devices can also encourage healthy behavior by providing incentives, reminders, and feedback to individuals, such as staying active, hydrating, eating healthily, and maintaining a healthy lifestyle by measuring hydration biomarkers and nutrients. In addition, they can significantly reduce healthcare costs by reducing the number of hospitalizations and emergency room visits, which can be expensive for both individuals and the healthcare system. Wearable technology enables remote monitoring of patients and personalized care.
Further recommendations will be available to the patients through AI algorithms on an individual’s diet and exercise habits. These tailored suggestions aim to improve overall health and reduce the risk of chronic diseases.[4]
Challenges for Wearables in Healthcare
· Accurate and Reliable Data Collection
· Inherent Limitations of Sensors
· Lack some features
· Dwindling Ergonomics
· User Privacy, Security, Cyber Risks and Hacking
· Water Proofing
· Interoperability Challenges
· Mostly Expensive
Despite the potential benefits of wearable health technology, there are several shortcomings, such as the accuracy and reliability of the data collected by these devices. As the biosensors are still in the development stage in monitoring biochemical signals, the technology is yet to sense biological biomarkers continuously, and they need to achieve higher sensitivity, selectivity, and accuracy towards specific biomolecule sensing. There is still a risk of inaccurate readings, which can lead to false alarms or missed opportunities for early detection of health issues. Another challenge is that of privacy and security concerns. When using wearable technology to collect and transmit sensitive health data, there is a risk of data breaches and unauthorized access to personal information. Healthcare providers and device manufacturers must ensure appropriate and extra care.[5]
Integration of AI is revolutionizing the accuracy and efficiency of wearable sensors by identifying and correcting errors in the collected data. AI algorithms can be used to analyze the massive amount of data collected by wearable devices, enabling healthcare providers to identify patterns, predict health outcomes, and make knowledgeable decisions about patient care. For instance, by examining an individual’s activity level, sleep patterns, and heart rate, AI algorithms can forecast the likelihood of heart attacks or strokes, empowering healthcare providers to take proactive measures. Another critical challenge in wearable sensor networks is managing their energy consumption, particularly when using wireless sensor networks (WSN), due to the often non-replaceable or rechargeable nature of sensor batteries. Efficient energy usage is deemed imperative, necessitating a thoughtful and optimal design of the WSN and sensor routing.[5]
Wearable Tech Has Transformed The Healthcare Industry
Photo by Chino Rocha on Unsplash
The healthcare industry has been a slow adopter of technology applications mainly due to its fragmented and highly complex systems. However, with the advent of Internet of Things (IoT), wearable technology and smart connected devices, patients get an opportunity to take charge of their health and act upon it. Healthcare providers no longer remain custodians of patient information and can positively influence patients to enhance engagement and health outcomes. While current sensor-based IoT devices in health are primarily in the area of wellness/activity tracking, remote diagnostics and chronic disease management, ingestible and contactless sensors that can sense odor, electromagnetic activity, are commercially available. This has the potential to provide a lot of value to increase transparency and efficiency in the healthcare system thereby reducing overall costs.
Portable Devices
From the early 21st century, wearable devices have begun to provide personalized health services, as well as advanced levels of personalized portable devices and sensors. Currently, portable devices nanomaterials can be classified as
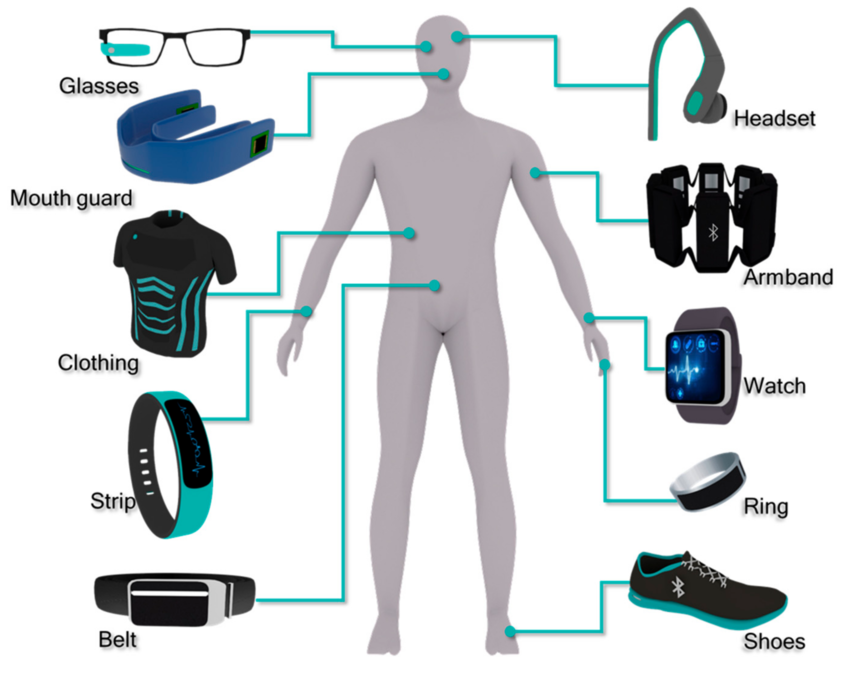
· Wrists (watches, bracelets and gloves),
· Heads (glasses and helmets),
· E.Textile-Body clothes (coats, underwear and pants),
· Others: Feet, and Body sensory control devices (somatosensory modulators).
Due to the miniaturization of biosensing devices, and the development of microelectronics and wireless communication technologies, the wearable monitoring systems deeply embedded in people’s lives have been further developed.
· Wrist-Mounted Devices: Wrist-mount devices for physiological monitoring have been developed commercially with improvement in battery longevity and miniaturization of hardware for converting raw signals to real-time interpretable data. Wrist-mounted devices, such as fitness bands and smart watches, are moving from basic accelerometer-based “smart pedometers” to include biometric sensing. Typical noninvasive monitoring devices carry out two functions: (1) communication with electronic devices and (2) monitoring of human physiological signals and human activity signals. Blood pressure measurement is one of the most important physiological indicators of an individual’s health status. Conventional pulse wave sensors used cuffs to non-invasively monitor blood pressure and included optical, pressure, and electrocardiogram (ECG) sensors. However, these sensors are large in size, difficult to handle, and cannot be accurately measured when the subject moves during blood pressure measurement. Smart watches are one of the most popular wearable device types, and GlucoWatch is the first to have a commercially approved non-invasive glucose monitor by the Food and Drug Administration (FDA). For monitoring of Parkinson’s disease (PD) patients, the smart watches can be used to analyze tremor and balance dysfunction with a gyroscope or accelerometer.
· Head-Mounted Devices: Wearable smart glasses are a type of head-mounted computer that displays information. Smart glasses are pulse-sensing glasses containing a sensor on the nose pad to continuously monitor heart rate.
· E-Textiles: Smart textiles, or smart clothing, consists of conductive devices and clothing material that is attached to or woven with the conductive devices. Textile-based diagnostic devices incorporate sensors, such as electrodes and fabrics, or by sewing electrodes into fabric. The integrated sensors into textiles have been used to analyze biofluids. Smart textiles must include three components. i.e a sensor, an actuator and a controlling unit. Textile containing electrodes, called e-textiles, are used to monitor human physiological signals, biomechanics and physical activity, such as motion, body acceleration and pressure. To measure glucose and lactate with high accuracy, some companies fabricated a glucose and lactate detection system by using glucose oxidase and lactate oxidase-based electrodes in a fabric. Physiological signals, such as heart rate, breathing rate and temperature, are also monitored using e-textiles. A wearable vest is capable of monitoring heart rate and breathing rate during daily activity.
· Others: An electronic shoe has been developed to measure walking ability, which provide fundamental information for distinguishing among gait phases. Smart jewelry such as a necklace, a bracelet, or clip, a wearable real-time monitoring device, is designed to warn users through smartphone alerts can track human activity, such as consumed calories and distance travel, and measure quality and duration of sleep. It detects sleep, daily activities, menstrual cycles, and breathing, and do not have commonly used sensors like GPS or a heart rate monitor. The smart belt monitor information such as waist size, food intake and movement of users like step count, and sitting time. As a smart chest strap, has monitoring electrodes providing information of electrocardiogram (ECG) and direct current for assessing the activity of the cardiac system and central nervous system. Another chest strap that features reliable real time recording of heart rate, breathing rate, temperature, ECG and respiratory rate. In particular, respiratory rate is detected by measuring chest expansion and contraction
Attachable Devices
Attachable monitoring devices are considered to be the next-generation personal portable health care devices for remote medical progression. An important feature that defines an attachable device is skin-like adaptability and flexibility, providing accurate and reliable sensing without compromising a user’s natural movement and comfort. Smart attachable sensing devices are an important component in real-time health monitoring systems for physiological signals that are closely associated to physical conditions such as blood pressure, heart rate, electrophysiology, body temperature and various sweating biomarkers.
· Wearable Skin Patches: Wearable skin patches are becoming increasingly pervasive within the wearables market. Soft, flexible and stretchable electronic devices are connected to soft tissue to provide a new platform for robotic feedback and control, regenerative medicine and continuous healthcare. Skin patches are ideal wearables, because they can be obscured by clothing, and can record more accurate data without being disturbed by movement. Wearable patches worn on the human skin have been utilized as cardiovascular, sweat, strain and temperature sensors.
Photo by Robina Weermeijer on Unsplash
· Monitoring of Blood Pressure and Heart Rate: Monitoring cardiovascular signals such as blood pressure and the heart rate of patients receiving medical care is very important. A wearable patch sensor for cuffless blood pressure monitoring has been developed. The system simultaneously measures epidermal pulse signals and the ECG and obtains bit-to-bit blood pressure data in real time. The wearable pulse wave monitoring sensor is attached directly to the epidermis, and the fluctuations of the pulse wave for a real-time arterial pulse monitoring system The developed sensor connected with a wireless blue-tooth transmitter and an Android-based smart phone which could display the detected signals in real time.
· Monitoring of Bodily Fluids: As a typical body fluid, sweat is especially important because it contains large amounts of important biomarkers, including electrolytes, small molecules, and proteins. Over the past few years wearable sensors have been developed for sweat analysis and have detected various sweat components. In order to reduce the negative effects of psychological stress upon human society and health, psychological stress should be constantly monitored in daily life. Therefore, researchers have developed a flexible human stress monitoring patch that can track skin temperature, skin conductance, and pulse waves.
· Contact Lens: Smart contact lenses can monitor the physiological information of the eyes and of any tears non-invasively. Several types of contact lenses using optical and electrical methods have been developed to monitor the chemicals (lactate and glucose) and electrical conductivity of the tear fluid and the transcutaneous gases in the eye’s mucous membrane. A wearable contact lens optical sensor has been developed to continuously measure glucose in physiological conditions.
Implantable and Ingestible Devices
Implantable or implanted devices have recently become an emerging measurement of wireless medical measurement. Since these devices operate directly in the body, they should be prevented in advance from adverse effects (such as rejection of transplantation) that may affect the human body. Insertion-type instruments are used to diagnose and treat diseases by detecting changes in the body, and ingested instruments are considered to be suitable for endoscopy because they pass through the digestive system.
· Implantable Devices: Since cardiac pacemakers were first developed in the 1960s, the number of patients treated with cardiovascular implantable electronic devices, including pacemakers, implantable cardiovascular defibrillators (ICDs) and implantable deep brain stimulators, has been increasing. The pacemaker is used to treat irregular heartbeats known as arrhythmias, and provides low-energy electrical pulses to restore normal rhythm when irregular heartbeats are detected. The ICD is the latest version of the pacemaker that operates in the same manner. Sudden cardiac death (SCD) accounts for half of all deaths from heart disease. If a conventional pacemaker is not able to restore normal rhythm to heart rate, an ICD will provide a high-energy electrical pulse; indeed, the ICD is associated with significant reductions in mortality among patients at high risk of SCD from ventricular arrhythmias. Deep brain stimulation has been introduced as an effective means of treating movement disorders such as Parkinson’s disease. Tattoos are fascinating platforms for monitoring emotions and vital signs. Electronic tattoos (e-tattoos) can be adapted to various skin textures, enabling noninvasive and best attachment methods to the skin. The texture of the tattoo adhesive layer is thoroughly flexible to move with any skin movement, providing natural wearability for the patient and precise data to the physician. Currently, electronic tattoos function as a means of diagnostic and monitoring for primary healthcare providers who want optimum clinical decisions to monitor the patient’s blood glucose levels.
· Ingestible Pills: A safe, non-invasive approach to accessing the fluid one wants to identify is to use an ingestible sensor. This ingestible sensor is able to pass through the lumen of the digestive tract and reach organs around the abdomen. Thus, the ingestion sensor monitors the intrinsic genital contents and luminal fluid as well as enzymes, hormones, electrolytes, microbial communities and metabolites around the organs and delivers biometric information. Ingestible pills, are smart pills for monitoring the precise time at which any drug is taken. When the smart pill reaches the stomach, it is powered up by a chemical reaction with the stomach fluid and sends an ingestion time signal to the patch worn on the body. This patch not only communicates with the smart pill, but also monitors heart rate, blood pressure, pH and temperature. The device can be controlled in real time with respect to drug intake information and compliance.
Current Market Situation
The available products are smart watches, wristbands, and patches. Few examples include smartwatches from Apple or Samsung, and fitness trackers from Fitbit. Such devices are designed to monitor various physiological parameters in the human body. There are also commercial wearable sensor designs in the form of clothing for monitoring various physiological parameters, tracking muscle activity, and monitoring posture.
Future Prospects, Outlook And Challenges
Recent developments in miniaturization of electronic devices, affordability, ergonomics, connection with smartphones, and easy usability can be counted as the reasons for the increased interest in wearable sensors in recent years. In addition, developments in wearable sensor technology are increasing due to reasons such as increasing health awareness and developments. The future of healthcare wearables is marked by several exciting trends and predictions. Advancements in sensor technology and AI are expected to further enhance the capabilities of wearable medical devices, making them more accurate and capable of monitoring a wider range of health metrics. The future of wearable technology in healthcare is promising, with emerging trends such as smart clothing, advanced sensors, and augmented reality. These technologies have the potential to revolutionize healthcare by enabling more accurate and personalized diagnosis and treatment of medical conditions. A 10.7% compound annual growth rate (CAGR) is forecast for wellness and fitness wearables from 2022 to 2030. A higher 14.3% CAGR is expected for the segment of headwear and eyewear products between 2022 and 2030. The growth of the global wearable technology market is predicted at 13.89% throughout the 2022 to 2030 forecast period.[9]
Wearable devices are becoming popular in various fields, from healthcare to biomedical monitoring systems. In particular, wearable devices are becoming important for long-term health monitoring due to the increasing elderly population throughout the world. Certain technical challenges still need to be addressed for the wide-scale use and deployment of wearable devices as part of the digital health era. One such technical challenge is the personal calibration of wearable devices. The symptoms for early disease diagnosis may differ for every person because every person is unique, and various factors can affect personal health (e.g., family medical history, genetics and diet). Therefore, using a wearable device to monitor a patient’s health more accurately and properly requires a machine-based analysis of personal data and a personal calibration of the device. Another challenge is the misalignment of wearables, which affects the quality and accuracy of the measurements.
References
1. Kim, J.; Campbell, A.S.; De Ávila, B.E.-F.; Wang, J. Wearable biosensors for healthcare monitoring. Nat. Biotechnol. 2019, 37, 389–406.
2. J. Kim et al. Wearable biosensors for healthcare monitoring Nat. Biotechnol. (2019)
3. Ajami, S. & Teimouri, F. Features and application of wearable biosensors in medical care. J. Res. Med. Sci. 20, 1208–1215. https://doi. org/ 10. 4103/ 1735- 1995. 172991(2015).
4. Ha, M., Lim, S. & Ko, H. Wearable and flexible sensors for user-interactive health monitoring devices. J. Mater. Chem. B.6, 4043–4064 (2018).
5. Wearable Sensors Market Worth $2.86 Billion by 2025 | CAGR: 38.8%. Available online: http://www. webcitation.org/73HUXmOKl (accessed on 19 October 2018).
6. Pantelopoulos, A.; Bourbakis, N.G. A survey on wearable sensor-based systems for health monitoring and prognosis. IEEE Trans. Syst. Manand Cybern. Part C (Appl. Rev.) 2010, 40, 1–
7. Chan, M.; Esteve, D.; Fourniols, J.Y.; Escriba, C.; Campo, E. Smart wearable systems: Current status and future challenges. Artif. Intell. Med. 2012, 56, 137–156.
8. Kim, J.; Campbell, A.S.; de Ávila, B.E.; Wang, J. Wearable biosensors for healthcare monitoring. Nat. Biotechnol. 2019, 37, 389–406.
9. Piwek L, et al. The rise of consumer health wearables: promises and barriers. PLOS Med. 2016;13(2):e1001953.