Lung Cancer and Women
Photo by Lukas Menke on Unsplash
The lungs are two spongy organs in the chest that control breathing. Lung cancer is a kind of cancer that starts as a growth of abnormal cells in the lungs. Lung cells divide and make more copies of themselves as a part of their normal function. But sometimes, they get changes (mutations) that cause them to keep making more of themselves when they shouldn’t. Damaged cells dividing uncontrollably create masses, or tumors, of tissue that eventually keep some organs from working properly.[1]
Lung cancer usually forms in tissues of the lung, usually in the airways (bronchi or bronchioles) or small air sacs (alveoli). Lung cancer often spreads to other parts of the body including brain and the bones. Once lung cancer has spread beyond the lungs, it's generally not curable. Lung cancer is the name for cancers that start in the lungs whereas the cancers that start in other places and move to the lungs are usually named for where they start. [1]
Types Of Lung Cancer
Mainly two main kinds: non-small cell lung cancer and small cell lung cancer. Of the main types, small cell lung cancer tends to spread faster than non-small cell lung cancer. By the time lung cancer is found, it may have already started spreading to lymph nodes or other organs:[2]
· Non-small cell lung cancer (NSCLC)- It accounts for over 80% of lung cancer cases. Common types include adenocarcinoma and squamous cell carcinoma. Adenosquamous carcinoma and sarcomatoid carcinoma are two less common types of NSCLC.
· Small cell lung cancer (SCLC)- This type grows more quickly and is harder to treat than NSCLC. It’s often found as a relatively small lung tumor that’s already spread to other parts of the body. Specific types of SCLC include small cell carcinoma (also called oat cell carcinoma) and combined small cell carcinoma.
· Other types of cancer in the lungs- including lymphomas (cancer in lymph nodes), sarcomas (cancer in bones or soft tissue) and pleural mesothelioma (cancer in the lining of lungs). These are treated differently and usually aren’t referred to as lung cancer.
Stages Of Lung Cancer
Cancer is usually staged based on the size of the initial tumor, how far or deep into the surrounding tissue it goes, and whether it’s spread to lymph nodes or other organs. The general staging for lung cancer is: [3]
· Stage 0 (in-situ): Cancer is in the top lining of the lung or bronchus. It hasn’t spread to other parts of the lung or outside of the lung.
· Stage I: Cancer hasn’t spread outside the lung.
· Stage II: Cancer is larger than Stage I, has spread to lymph nodes inside the lung, or there’s more than one tumor in the same lobe of the lung.
· Stage III: Cancer is larger than Stage II, has spread to nearby lymph nodes or structures or there’s more than one tumor in a different lobe of the same lung.
· Stage IV: Cancer has spread to the other lung, the fluid around the lung, around the heart or distant organs.
Metastatic lung cancer is cancer that starts in one lung but spreads to the other lung or to other organs. Metastatic lung cancer is harder to treat than cancer that hasn’t spread outside of its original location.
Lung Cancer Prevalence
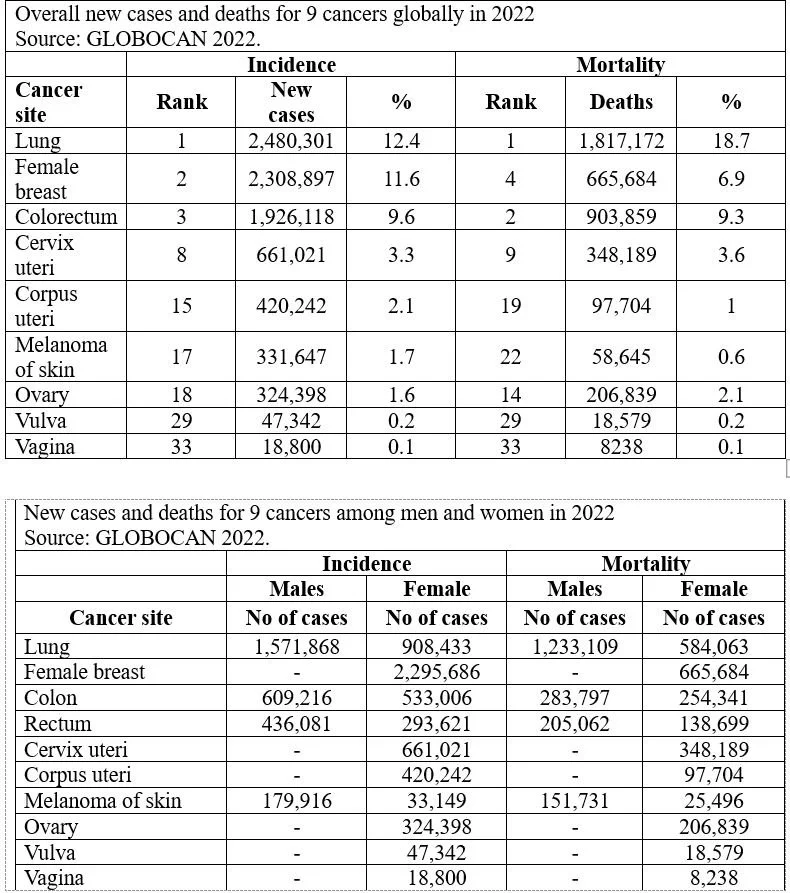
Lung cancer is the third most common cancer globally. Health systems report over 2,480,301of new cases of lung cancer each year. [3]
These figures present global cancer statistics by world region for the year 2022 based on updated estimates from the International Agency for Research on Cancer (IARC). There were close to 2.4 million new cases of cancer in the year 2022 alongside 9.7 million deaths from cancer. The estimates suggest that approximately one in five men or women develop cancer in a lifetime, whereas around one in nine men and one in 12 women die from it. Overall, the chance that a man will develop lung cancer in his lifetime is about 1 in 16; for a woman, the risk is about 1 in 17. Lung cancer was the most frequently diagnosed cancer in 2022, responsible for almost 2.5 million new cases, or one in eight cancers worldwide (12.4% of all cancers globally), followed by cancers of the female breast (11.6%), colorectum (9.6%). Lung cancer was also the leading cause of cancer death, with an estimated 1.8 million deaths (18.7%), followed by colorectal (9.3%), and female breast (6.9%) cancers. Breast cancer and lung cancer were the most frequent cancers in women and men, respectively (both cases and deaths). With demographics-based predictions indicating that the number of new cases of cancer will reach 35 million by 2050, investments in prevention, including the targeting of key risk factors for cancer (including smoking, overweight and obesity, and infection), could avert millions of future cancer diagnoses and save many lives worldwide, bringing huge economic as well as societal dividends to countries in the forthcoming decades. [3]
Symptoms
Lung cancer typically doesn't cause symptoms early on. Symptoms of lung cancer usually happen when the disease is advanced. Signs and symptoms of lung cancer that happen in and around the lungs may include: [3]
· A recent cough that doesn't go away.
· Chest pain.
· Coughing up blood, even a small amount (hemoptysis).
· Hoarseness.
· Shortness of breath.
· Wheezing.
· Unexplained fatigue (tiredness).
· Shoulder pain.
Signs and symptoms that happen when lung cancer spreads to other parts of the body may include:
· Bone pain.
· Headache.
· Losing weight without trying.
· Loss of appetite.
· Swelling in the face or neck.
· Shoulder pain.
· Swelling in the arms or upper chest (superior vena cava syndrome).
· Small pupil and drooping eyelid in one eye with little or no sweating on that side of the face (Horner’s syndrome).
Causes
Lung cancer happens when cells in the lungs develop changes in their DNA. A cell's DNA holds the instructions that tell a cell what to do. In healthy cells, the DNA gives instructions to grow and multiply at a set rate and also to die at a set time. In cancer cells, the DNA changes give different instructions. The changes tell the cancer cells to make many more cells quickly. Cancer cells can keep living when healthy cells would die. This causes too many cells.
The cancer cells might form a mass called a tumor. The tumor can grow to invade and destroy healthy body tissue. In time, cancer cells can break away and spread to other parts of the body called metastatic cancer. [3]
Risk Factors
A number of factors may increase the risk of lung cancer. Some risk factors can be controlled, for instance, by quitting smoking. Other factors can't be controlled, such as family history. Risk factors for lung cancer include: [4]
· Smoking- Risk of lung cancer increases with the number of cigarettes one smokes each day which increases with the number of years smoked. Smoking any kind of tobacco products, including cigarettes, cigars or pipes estimate 80% of lung cancer. Quitting at any age can significantly lower the risk of developing lung cancer. Vaping (a device to inhale a mist of nicotine and flavoring), including some that are known to cause cancer has the potential to cause lung damage.
· Exposure to secondhand smoke- Even if one doesn't smoke, the risk of lung cancer increases if people around are smoking called secondhand smoke.
· Previous radiation therapy- Having previous radiation treatments to chest (for instance, for breast cancer or lymphoma may have an increased risk of developing lung cancer.
· Exposure to radon gas- Radon is produced by the natural breakdown of uranium in soil, rock and water. Radon eventually becomes part of the air one breathes. Unsafe levels of radon can build up in any building, including homes.
· Exposure to cancer-causing substances- Workplace exposure to cancer-causing substances, called carcinogens, can increase risk of developing lung cancer. The risk may be higher if one smokes. Carcinogens linked to lung cancer risk include asbestos, arsenic, chromium and nickel, diesel exhaust, silica, coal products and others.
· Family history of lung cancer- People with a parent, sibling or child with lung cancer have an increased risk of the disease.
Photo by National Cancer Institute on Unsplash
Diagnosis and Tests
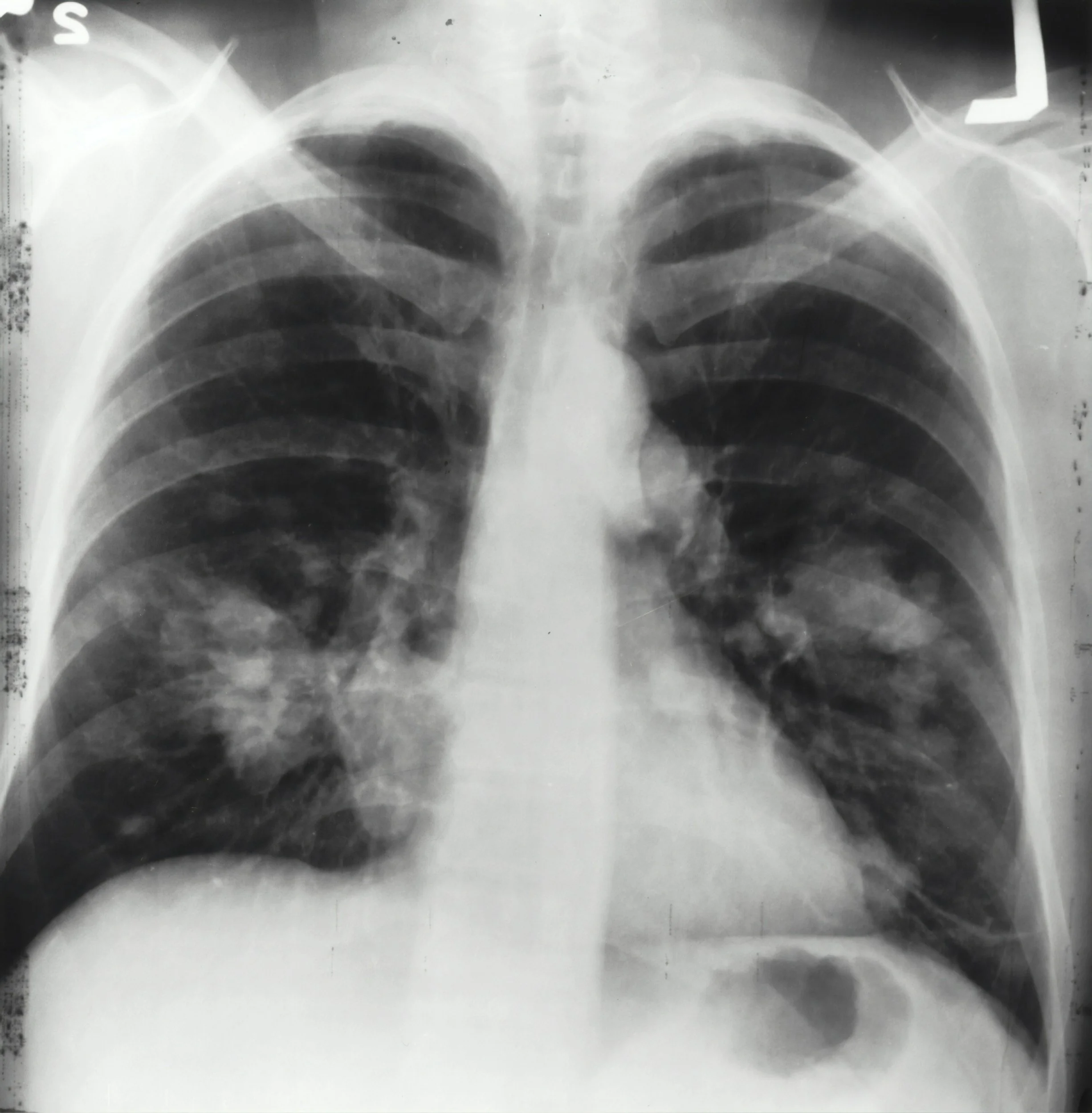
Diagnosing lung cancer can be a multi-step process. It usually involves history taking, listening to symptoms, performing a physical exam and getting blood tests and a chest X-ray. [5]
If lung cancer is suspected, next steps in diagnosis would usually involve more imaging tests like PET/CT scan to see if cancer has spread, and tests of cancerous tissue from a biopsy.
· Chest X-ray: X-rays can’t diagnose lung cancer — they can only show if there’s something suspicious that they should look into further.
· Blood tests: can help health provider check how organs and other parts of body are working.
· Imaging: Chest X-rays and CT scans provide images that can show changes in lungs. PET/CT scans are usually done to evaluate a concerning finding on a CT scan or after a cancer diagnosis to determine whether cancer has spread.
· Biopsy: There are a number of procedures which can be used to look more closely at what’s going on inside the chest. During the same procedures, the doctor can take samples of tissue or fluid (biopsy), which can be studied under a microscope to look for cancer cells and determine what kind of cancer it is. Samples can also be tested for genetic changes (mutations) that might affect the treatment.
Procedures used to initially diagnose lung cancer or learn more about its spread include:
· Needle biopsy:. During this procedure, a needle is used to collect samples of fluid or tissue.
· Bronchoscopy, thoracoscopy or video-assisted thoracic surgery (VATS): These procedures are used to look at parts of lungs and take tissue samples.
· Thoracentesis: used to take a sample of the fluid around lungs for testing.
· Endobronchial ultrasound or endoscopic esophageal ultrasound: A procedure to look at and biopsy lymph nodes.
· Mediastinoscopy or mediastinotomy: A procedure to look at and take samples from the area between the lungs (mediastinum).
· Molecular tests: As part of a biopsy, the health providers might have the tissue sample tested for gene changes (mutations) that special drugs can target as part of treatment plan. Genes that might have changes that can be targeted include: KRAS,BRAF,RET,MET, HER2, NTRK and many others.
Management and Treatment
Treatments can remove cancerous cells, help to destroy them or keep them from multiplying or teach the immune system to fight them. Some therapies are also used to reduce symptoms and relieve pain. The treatment will depend on the type of lung cancer, where it is, how far it’s spread and many other factors. [6]
Lung cancer treatments include surgery, radiofrequency ablation, radiation therapy, chemotherapy, targeted drug therapy and immunotherapy.
· Surgery- Cancer that hasn’t spread and limited to a single tumor can be eligible for surgery. The surgeon might remove the tumor and a small amount of healthy tissue around it to make sure they don’t leave any cancer cells behind. Sometimes they have to remove all or part of lung (resection) for the best chance that the cancer won’t come back.
· Radiofrequency ablation- Tumors near the outer edges of lungs are sometimes treated with radiofrequency ablation (RFA). RFA uses high-energy radio waves to heat and destroy cancer cells.
· Radiation therapy- uses high energy beams to kill cancer cells. It can be used by itself or to help make surgery more effective. Radiation can also be used as palliative care, to shrink tumors and relieve pain.
· Chemotherapy- is often a combination of multiple medications designed to stop cancer cells from growing. It can be given before or after surgery or in combination with other types of medication, like immunotherapy. Chemotherapy for lung cancer is usually given through an IV.
· Targeted drug therapy- In some people, lung cancer cells have specific changes (mutations) that help the cancer grow. Special drugs target these mutations to try to slow down or destroy cancer cells. Other drugs, called angiogenesis inhibitors, can keep the tumor from creating new blood vessels, which the cancer cells need to grow.
· Immunotherapy- Human bodies usually recognize cells that are damaged or harmful and destroy them. Cancer has ways to hide from the immune system to keep from being destroyed. Immunotherapy reveals cancer cells to immune system so the own body can fight cancer.
· Treatments to ease symptoms (palliative care)-Some lung cancer treatments are used to relieve symptoms, like pain and difficulty breathing. These include therapies to reduce or remove tumors that are blocking airways, and procedures to remove fluid from around your lungs and keep it from coming back.
Prevention
There's no sure way to prevent lung cancer, but one can reduce risk if people: [7]
· Don't smoke- Begin conversations about the dangers of smoking with family members early so that they know how to react to peer pressure.
· Stop smoking- Quitting reduces risk of lung cancer, even if one has smoked for years. Options include nicotine replacement products, medicines and support groups.
· Avoid secondhand smoke- If one lives or work with a person who smokes, urge them to quit or ask them to smoke outside. Avoid areas where people smoke, such as bars. Seek out smoke-free options.
· Test home for radon- High radon levels can be fixed to make home safer. Radon test kits are often sold at hardware stores and can be purchased online.
· Avoid carcinogens at work- Take precautions to protect from exposure to toxic chemicals at work like face mask for protection.
· Eat a diet full of fruits and vegetables- Choose a healthy diet with a variety of fruits and vegetables. Food sources of vitamins and nutrients are best
· Exercise - If you don't exercise regularly, start out slowly. Try to exercise most days of the week.
Lung cancer screening
One is eligible for lung cancer screening if he/she meets all of these requirements:
· Between the ages of 50 and 80.
· Currently smoker or have quit smoking within the last 15 years.
· If have a 20 pack-year smoking history (number of packs of cigarettes per day times the number of years one smoked).
Survival Rate Of Lung Cancer
The survival rate of lung cancer depends greatly on how far cancer has spread when it’s diagnosed, how it responds to treatment, overall health and other factors. For instance, for small tumors that haven’t spread to the lymph nodes, the survival rates are 90% for tumors that are smaller than 1 cm, 85% for tumors between 1 and 2 cm, and 80% for tumors between 2 and 3 cm. The relative five-year survival rate for lung cancer diagnosed at any stage is 22.9%.
A vast majority of lung cancer deaths are attributable to cigarette smoking, and curbing the rates of cigarette smoking is imperative. Understanding the epidemiology and causal factors of lung cancer can provide additional foundation for disease prevention. The role of tobacco as an etiologic factor in lung cancer has been convincingly established. Likewise, ionizing radiation and certain occupational exposures have been recognized as carcinogenic.
The absolute number of lung cancer cases continues to be alarming, with the continued rise of lung cancer in women a particularly disturbing feature. The challenge in
the future will be to modify the impact of these identified external sources of risk while continuing to expand knowledge of the genetic and molecular basis of carcinogenesis. Early diagnosis of lung cancer is imperative because the 5-year survival rate for treated stage I lung cancer is substantially better than for stages II to IV. Although work in the field of lung cancer treatment continues to be and remains important, the dismal survival rate associated with this disease demands that the medical profession contribute to efforts aimed at limiting its primary cause mainly tobacco smoking.
References
1. Herbst RS, Heymach JV, Lippman SM. Lung cancer. N Engl J Med. 2008; 359(13):1367–1380.
2. Christiani DC, Amos CI (2022). "Lung Cancer: Epidemiology". In Broaddus C, Ernst JD, King TE, et al. (eds.). Murray & Nadel's Textbook of Respiratory Medicine (7th ed.). Elsevier. pp. 1018–1028.
3. International Agency for Research on Cancer. GLOBOCAN Lung Cancer Facts Sheet 2020. Tindle HA, Stevenson Duncan M, Greevy RA, et al. Lifetime Smoking History and Risk of Lung Cancer: Results From the Framingham Heart Study. (https://pubmed.ncbi.nlm.nih.gov/29788259/) J Natl Cancer Inst. 2018 Nov 1;110(11):1201-1207. Accessed 10/31/2022.
4. U.S. Public Health Service, office of the Surgeon General: The health consequences of smoking. National Clearinghouse for Smoking Health. 1972
5. Pastis NJ, Gonzalez AV, Silvestri GA (2022). "Lung Cancer: Diagnosis and Staging". In Broaddus C, Ernst JD, King TE, et al. (eds.). Murray & Nadel's Textbook of Respiratory Medicine (7th ed.). Elsevier. pp. 1039–1051
6. Rivera P, Mody GN, Weiner AA (2022). "Lung Cancer: Treatment". In Broaddus C, Ernst JD, King TE, et al. (eds.). Murray & Nadel's Textbook of Respiratory Medicine (7 ed.). Elsevier. pp. 1052–1065.
7. Bade BC, Dela Cruz CS (March 2020). "Lung Cancer 2020: Epidemiology, Etiology, and Prevention". Clin Chest Med. 41 (1): 1–24. doi:10.1016/j.ccm.2019.10.001