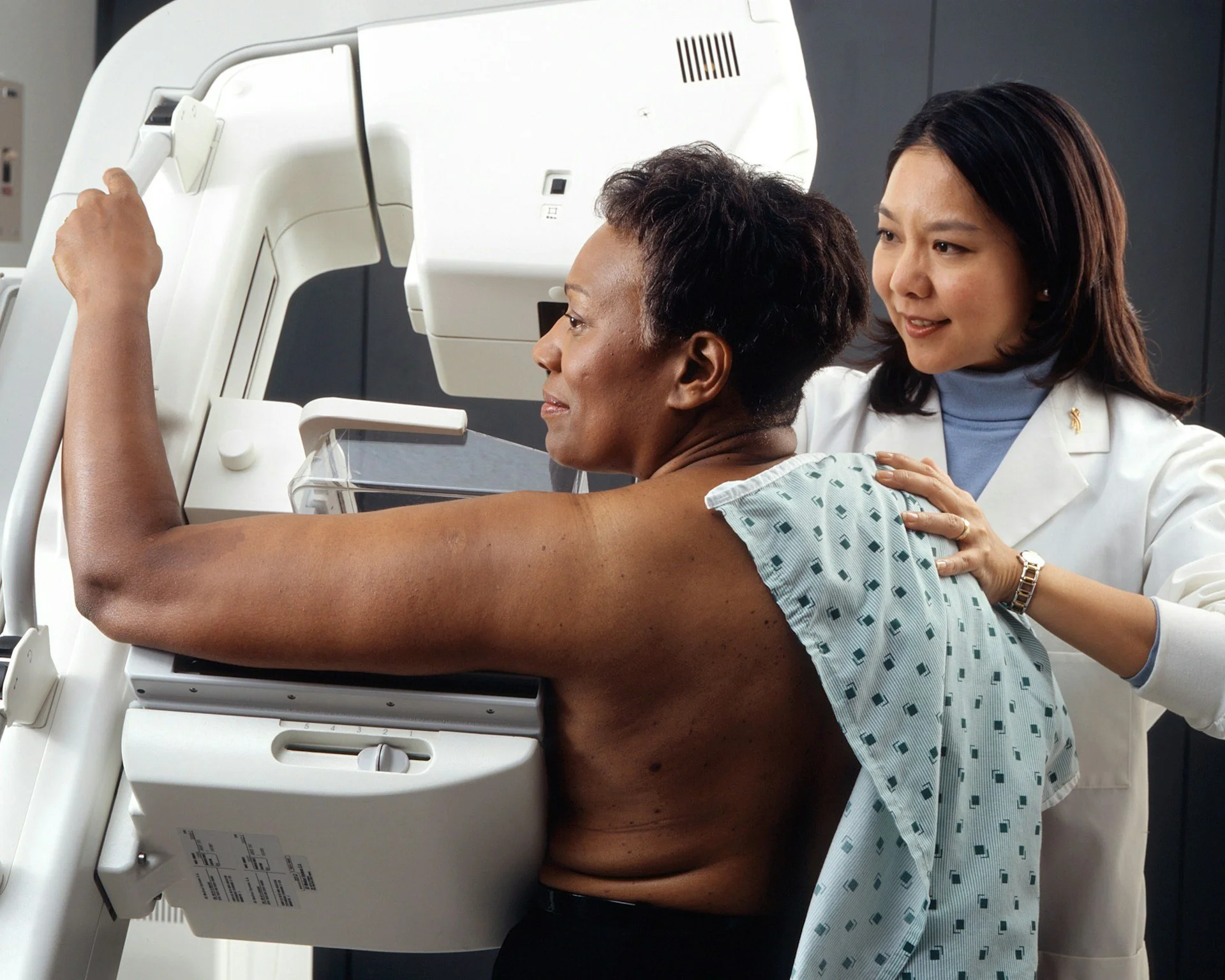
Understanding Breast Cancer - The Silent Killer
Breast a glandular organ (mammary gland) is made up of connective tissue, fat, and breast tissue that contains the glands to make milk. Breast cancers can start from different parts of the breast. It is a type of cancer that starts in one or both breasts. Breast cancer occurs almost entirely in women, but men can get breast cancer, too. Cancer starts when cells begin to grow out of control. It’s important to understand that most breast lumps are benign and not cancer (malignant). Non-cancer breast tumors are abnormal growths, and do not spread outside of the breast. Any breast lump or change needs to be checked by a health care professional to find out if it is benign or malignant (cancer) and if it might affect one’s future cancer risk.[1]
Breast cancer can spread when the cancer cells get into the blood or lymph system and then are carried to other parts of the body. If cancer cells have spread to the lymph nodes, there is a higher chance that the cells could have traveled through the lymph system and spread (metastasized) to other parts of the body. [1]
Major Causes/ Risk Factors Of Breast Cancer
· Gene Mutations: The normal breast cells can become cancer because of changes or mutations in genes. Only 10% cancers are linked with known abnormal genes that are passed on from parents (inherited). Most breast cancers (about 90%) develop from acquired (not inherited) genes. Breast cancer happens when cells in the breast change and grow out of control. The cells usually form a tumor (also called neoplasm, a mass of abnormal cells that form in body). Sometimes the cancer does not spread any further. This is called "in situ." If the cancer spreads outside the breast, the cancer is called "invasive." It may just spread to nearby tissues and lymph nodes.
Genes control how body cells function. They are made up of a chemical called DNA, which comes from both the parents. DNA affects more than just how one looks; it also can influence the risk for developing certain diseases, including some kinds of cancer. Normal cells have genes called proto-oncogenes, which help control when the cells grow, divide to make new cells, or stay alive. If a proto-oncogene is mutated (changed) in a certain way, it becomes an oncogene. Cells that have these mutated oncogenes can become cancer. Normal cells also have genes called tumor suppressor genes, which help control how often normal cells divide in two, repair DNA mistakes, or cause cells to die at the right time. If a cell has a mutated tumor suppressor gene, then the cell can turn into cancer. Cancers can be caused by gene changes that turn on oncogenes or turn off tumor suppressor genes.
· Inherited Gene Changes : Some gene changes (mutations) are inherited or passed to from parents. This means the mutations are in all cells when one is born. Certain inherited gene changes can greatly increase the risk for developing certain cancers and are linked to many of the cancers that run in some families. Some genes are tumor suppressor genes. When one of these genes changes, it no longer suppresses abnormal cell growth, and cancer is more likely to develop. A change in one of these genes can be passed from a parent to a child.
Genetic testing can identify some women who have inherited mutations in the genes. Since these mutations are also often associated with other cancers (besides breast), women with these mutations might also consider early screening and preventive actions for other cancers. The genes involved can affect things like hormone levels, metabolism, or other factors that impact risk for breast cancer. These genes might also cause much of the risk of breast cancer that runs in families.
· Acquired Gene Changes: Most gene mutations linked to breast cancer are acquired. This means the change takes place in breast cells during a person's life rather than having been inherited or born with them. Acquired DNA mutations take place over time. These acquired mutations of oncogenes and/or tumor suppressor genes may result from other factors, like radiation or cancer-causing chemicals etc.
· Lifestyle-Related Risk Factors: Certain factors increase the risk of breast cancer including increasing age, obesity, harmful use of alcohol, family history of breast cancer, history of radiation exposure, reproductive history (such as age that menstrual periods began and age at first pregnancy), tobacco use and postmenopausal hormone therapy. Breast cancer occurrence increases with age and peaks at menopause. Beginning menopause after the age of 55 years may increase exposure to estrogen (it is a steroid hormone associated with the female reproductive organs and is responsible for developing female sexual characteristics), which may increase the risk of breast cancer. Simply being a woman is the main risk factor for developing breast cancer. Although women have many more breast cells than men, the main reason they develop breast cancer more often is because their breast cells are constantly exposed to the female hormones estrogen and progesterone, which promote cell growth. The role of hormones in many cases of breast cancer, is not yet fully understood. [2]
Photo by National Cancer Institute on Unsplash
Prevalence Of Breast Cancer In Developed And Developing Countries
The incidence rate of breast cancer is higher in Western European countries as compared to Eastern Asian or African countries. However, survival rates are much higher in Western European countries as compared to low- and middle-income countries. This is attributed to the significantly better screening and treatment facilities prevalent in high-income countries. In addition, higher awareness about the timely screening of mammography in high income countries has reduced breast cancer mortality in the previous four decades.
The differences in incidence between countries can be attributed to changes in exposure to environmental risk factors, behaviour and lifestyle factors of the different population groups. In general, the high rates of breast cancer in developed countries are the consequence of a higher prevalence of the known risk factors for the disease, many of which – early age at menarche, nulliparity, late age at first birth, late age at any birth, low parity, and late menopause – relate to the hormonal imbalance. As life expectancy increases alongside economic development in these regions, one can expect to see an increase in breast cancer incidence. Other risk factors of importance can be classified into reproductive and non-reproductive factors, which are all influenced by economic development. Evidence shows that women living in marginalized areas have a higher risk of dying from preventable cancer deaths than other populations due to a combination of vulnerabilities that often result in late detection and delayed or incomplete treatment. Major vulnerabilities include lower socioeconomic status, less access to education, living in small rural communities that lack access to many services, including healthcare.[2]
Perceived Barriers To Early Breast Cancer Diagnosis
Women generally in underdeveloped countries lack appropriate awareness about diagnosis and treatment for breast cancer due to a range of following multifaceted barriers[3]
· Social And Cultural Context Barriers: Generally, women in conservative societies hesitate to expose breast cancer as these are considered as sensitive parts of a woman’s body which have to be concealed all the time. Breast cancer patients delay their medical treatment because of distress in discussing the breast-related problems in front of a male physician. Women desire modesty and respect for their privacy and that is the major barrier for screening and treatment of breast cancer.
· Lack Of Cancer Awareness: Majority of women in underdeveloped countries do not have knowledge of breast screenings, self-examination, treatment facilities when they first observe lump in their bodies.
· Myths And Beliefs : In societies where people follow religious beliefs, they often associate calamities and afflictions with the will of God and believe that supernatural interventions can cure the disease. Breast cancer is considered a contagious disease by family members, most of whom choose to avoid breast cancer patients. Women face a plethora of emotional problems after diagnosis including: isolation, employment issues, stress, blame of bad luck, and social critique. In addition, the fear that breast cancer reflects upon the bad character of women, shyness, and fear of husband’s separation also contribute to hiding and delay in breast cancer screening.
· Traditional Medicine Use: Lack of knowledge about appropriate breast cancer screening and treatment can cause negative perceptions and their unrealistic reliance on spiritual and traditional treatment. In such a situation, patients prefer to seek alternative treatment such as to visit the shrines or religious leaders (faith healers), and traditional healers instead of attending hospitals. In traditional societies it has also been found that women initially seek spiritual treatment until their tumor starts growing. Furthermore, women who belong to lower socioeconomic class mostly avoid attending hospitals due to prohibitive distances, travel costs, and treatment expenses and use holy water and Taweez (amulet) to cure the disease.
· Lack Of Social Support: Generally breast cancer patients are not provided with appropriate social support due to older age, the severity of cancer treatment, and co-morbidities. Majority of patients themselves evade available social support from family members and friends, because of providers’ gazes which negatively impact patient’s self-esteem and due to possible sympathy. The cancer stigma causes disruption to interaction with ‘normal’ among cancer patients.
· Fear Of Cancer: Patients are fearful of treatment side effects such as: hairlessness and the loss of eyebrows and eyelashes. They feel that these changes would disfigure their body image. They purposely delay their treatment due to the fear of mastectomy and loss of femininity “being a woman without breasts” through seeking advance medical treatment. Breast cancer treatments often result in serious changes in the appearance of patients, including breast asymmetry and changes in skin texture and sensitivity. Women do not disclose their disease to avoid social stigma and are reluctant for screening.
· Discrimination/Mistreatment By Health Care Personnel: It may be a consequence of healthcare ethnic and gender discrimination resulting in the provision of unequal healthcare and disparities in cancer outcomes. In turn, these experiences of mistreatment and discrimination, damage the patients’ trust in healthcare providers, and thus, can act thereafter as barriers to participation in screening, timely healthcare seeking and adherence to treatment. Language barriers, long waiting times and difficulties in making an appointment are some other barriers.
· Cancer Stigma: In some cultures, discussion of female anatomy may be a taboo or awkward topic, where breasts are considered private organs not to be discussed in public. Reluctance to talk about cancer in their community and own families, women with breast cancer generally do not reveal their diagnosis. Cancer in general is viewed as a fatal disease, which majority of females associate with death, pain, suffering and aggressive treatments. Therefore, if they think their symptoms are related with cancer, they are likely to postpone seeking medical care in order to avoid what they see as aggressive unnecessary treatments.
· Costs/Distance To Health Services: In underdeveloped countries screening and treatment facilities are scarce and expensive and patients usually avoid seeking care due to lack of money. Having to cover costs of medical care is a major barrier in private service use. Even if they manage to get a consultation in public services without having to pay, they often can’t cover the costs of the medicines. In addition to direct medical costs, there are costs related to transportation and time.
Facilitators To Timely Healthcare Seeking
Following are considered as facilitators for early breast cancer diagnosis and treatment: - [4]
· Socio-Cultural Level: People find informative posters in the community and community health workshops very useful to keep themselves informed on the importance of taking care of their health. The messages and information received through the media (radio and television commercials), social networks, and screening mammography promotion activities done in their communities also help in enhancing awareness.
· Health Services Organization- Respectful patient-centered medical care would facilitate early cancer diagnosis and medical attention as patients will be receiving empathetic care with good attitudes of healthcare personnel and effective communication between doctors and patients.
· Information By Doctors And Promoters- Women should receive information about breast cancer by health care personnel in public primary care clinics and private services about breast self-examination.
· Social Support: From other women and from their family members, especially their partners. One on one hearing experiences of women who had cancer could be a strong motivator for others to check themselves and go to the doctor.
· Improved Perception: Perceived benefits of early breast cancer detection increase the chances of cure, and this motivates the patients to keep themselves informed and to talk about it with their peers.
· Educational Interventions: To increase individuals’ knowledge, awareness, risk perception and motivation to seek healthcare, can be effective only if designed and tailored according to the needs, beliefs and cosmovision of the local population.
· Role Of Health Care Providers: It is imperative that clinics treating patients pay attention to the barriers experienced by respective segments. Failure to recognize the cultural beliefs, ethnic taboos, and scientific misconceptions in individual patient can doom the success of cancer care programs, even if adequate resources are provided.
· Role At Government Level : Breast cancer burden can be managed, in low-, middle- and high-income countries, by enhancing healthcare systems, government collaboration to change public health policies and provide adequate diagnostic systems, creating awareness of the disease and implementing effective guidelines for diagnosis and treatment. Healthcare providers and policy makers should take notice of local women’s beliefs, access barriers and healthcare discrimination experiences in the design of programs that aim to facilitate early breast cancer diagnosis and treatment for these vulnerable populations.
Breast cancer constitutes an alarming burden worldwide that may rise due to an increase in growth and aging of population. In economically less developed countries, the frequency of breast cancer incidence in young women is rising. This burden is also influenced by a change of behaviour and lifestyle, which play a vital role in breast cancer development. There are multifaceted barriers to breast cancer diagnosis and treatment including individual, socio-cultural and structural including: lack of awareness, spiritual healing, and hesitance in accepting social support; feminine sensitivity, stigmatization; aversion to male doctors; lack of financial resources and apathetic medical system. Implementing a strategy to deal with psychological, socio-cultural, and structural barriers through cancer screening and treatment can be fruitful.
References
1. Saunders C, Jassal S (2009). Breast cancer (1. ed.). Oxford: Oxford University Press. p. Chapter 13. ISBN 978-0-19-955869-8.
2. Walsh MF, Cadoo K, Salo-Mullen EE, Dubard-Gault M, Stadler ZK and Offit K. Chapter 13: Genetic Factors – Hereditary Cancer Predisposition Syndromes. In: Niederhuber JE, Armitage JO, Doroshow JH, Kastan MB, Tepper JE, eds. Abeloff’s Clinical Oncology. 6th ed. Philadelphia, Pa: Elsevier; 2020.
3. Freeman HP, Chu KC. Determinants of cancer disparities: barriers to cancer screening, diagnosis, and treatment. Surg Oncol Clin. 2005;14(4):655–69.
4. Gakunga R, Kinyanjui A, Ali Z, Ochieng E, Gikaara N, Maluni F, et al. Identifying barriers and facilitators to breast cancer early detection and subsequent treatment engagement in Kenya: a qualitative approach. Oncologist. 2019;24:1549–56