Understanding the Global Shortage of Nurses and Doctors
Photo by Carlos Magno on Unsplash
A robust workforce is a sine qua non for any organization to operate productively to achieve its goals. More than two-thirds of the expenditure of an organization is consumed by human resources, besides the huge amount of time and other resources spent in terms of management. Successful and productive organizations are synonymous with effectively and efficiently managed human resources. Human resources have always remained the most important asset of any system or organization. Out of man, money, and material, man has always stood his ground as the strongest contender for making things happen. The objective of human resource planning is to ensure that the right number of personnel with the appropriate skills and competencies are available in the right place at the right time. Human resource planning is a critical activity within the broader sectoral planning activities.
Health services rely heavily on personnel, whereby 60–75% of the health sector budget is spent on sustaining this particular resource. According to WHO, Human resources for health (HRH) are identified as one of the core building blocks of a health system. They include physicians, nurses, midwives, dentists, allied health professionals, community health workers, social health workers, and other healthcare providers, as well as health management and support personnel – those who may not deliver services directly but are essential to effective health system functioning, including health services managers, medical records and health information technicians, health economists, health supply chain managers, medical secretaries, and others.[1] The World Health Organization (WHO) estimates that around 59.2 million health providers are working around the globe, and a shortage of almost 4.3 million physicians, midwives, nurses, and support workers worldwide as a result of decades of underinvestment in health worker education, training, wages, working environment, and management. The shortage is most severe in 57 of the poorest countries, especially in sub-Saharan Africa. Shortages of skilled health workers are also reported in many specific care areas. For example, there is an estimated shortage of 1.18 million mental health professionals, including 55,000 psychiatrists, 628,000 nurses in mental health settings, and 493,000 psychosocial care providers needed to treat mental disorders in 144 low- and middle-income countries. The developing world suffers greatly at the hands of the health workforce crisis. [2]
Globally the medical sector has largely been preoccupied with cure rather than care. The countries continue to produce a large number of doctors every year, ignoring the nursing workforce, which is critical for healthcare as the spinal cord is for the human body. Nurses have a lot of patients to take care of, but are insufficient in numbers to handle them.
Providing quality care is challenging when they’re stretched so thin. In developing countries, nursing faces a unique set of challenges that make it more difficult to provide quality care and attract people to the profession. Nurses are often perceived as assistants to doctors, which is a misconception. Nurses are highly educated professionals who complete rigorous training and licensing requirements to be able to practice. They also have to have the required experience and knowledge that is essential for patient care, and their contributions should be acknowledged. One of the biggest challenges the profession faces is the shortage of trained professionals. According to the World Health Organization (WHO), low, and middle-income countries will face a global shortage of 10 million health workers, including nurses, midwives, and doctors by 2030.[3] Untrained nurses lack the necessary knowledge and expertise to provide quality patient care, and they may not even be aware of their limitations. The professionals may lack the necessary communication and interpersonal skills to effectively interact with patients and their families. Patient care requires not only technical knowledge but also empathy and compassion, which untrained nurses may not possess. Moreover, practitioners opine that in many healthcare settings, nurses often take on additional responsibilities to ensure patients receive the care they need. This shortage has a significant impact on the quality of healthcare, thus making the nurses overwork and compromise on patient care. Professionals associated with the field say nurses are also asked to perform tasks that are outside of their scope of practice, such as performing procedures that require a physician’s expertise or making decisions that are typically reserved for doctors. The shortage of nurses globally is not a new issue, and a lack of funding and resources for nursing education programs has exacerbated it. The situation is further complicated by the low salaries and poor working conditions that deter qualified nurses from entering or remaining in the profession. To address the challenges faced by professionals in the country, it is very important to promote a positive image of nurses in the media. [4]
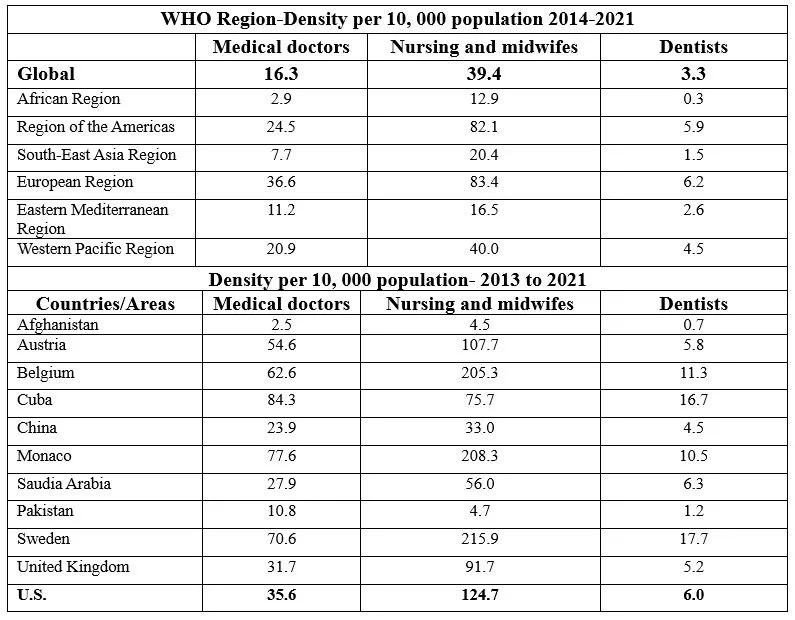
The statistics shown below are official WHO statistics for selected health-related SDG indicators and selected Thirteenth General Programme of Work indicators, based on data available in early 2023. An adequate health workforce is defined by WHO as at least 2.3 well-trained healthcare providers available per 1000 people and balanced in such a way as to reach 80% of the population or more with skilled birth attendance and childhood immunization.[4]
The Shortage of Healthcare Workers in the U.S.
The US healthcare industry is experiencing a severe shortage of workers at every level—a crisis worsened by the COVID-19 pandemic. The American Hospital Association estimates that the industry will face a shortage of up to 124,000 physicians by 2033. Meanwhile, it will need to hire at least 200,000 nurses a year to meet rising demands. Among support personnel, a shortage of home health aides is most acute. One study project predicts that if US workforce trends continue, more than 6.5 million healthcare professionals will permanently leave their positions by 2026, while only 1.9 million will step in to replace them, leaving a national industry shortage of more than 4 million workers.[5]
The American Association of Medical Colleges (AAMC) predicts that by 2025 there will be a shortage of as many as 122,000 physicians, more than 400,000 home health aides, and 29,400 nurse practitioners and other healthcare professionals. There is no easy solution to this problem. Healthcare workers need extensive training and specific qualifications, so providers cannot simply hire new workers off the street. There have been different responses and plans that seek to address healthcare worker shortages.[6]
Shortage Of Healthcare Professionals – Most-Affected Professions
Every type of medical professional is in short supply—including doctors, nurses, administrators, aides, assistants, and techs—but some professions are facing a more critical shortage than others. [6]
Physicians: Physician shortages vary by specialty. The biggest shortfalls tend to be in fields where compensation levels are relatively low while the rigors of the job are high. Infectious disease physicians, primary care doctors, and pediatricians, for example, tend to make less money and work longer, less predictable hours than dermatologists. Meanwhile, the aging population is starting to overwhelm the supply of cardiologists, orthopedic and vascular surgeons, neurologists, rheumatologists, pulmonologists, and other geriatric specialists, many of whom are aging out of their professions themselves. The AAMC projects a dramatic shortage of physicians in 2032. However, this shortage is even more problematic when one considers physician specialties which are often more lucrative and prestigious.
Nurses: Many nurses are reconsidering the profession because of burnout and insufficient pay. Others are moving on to seek career opportunities in new or related fields, such as consulting, insurance, teaching, or human resources. Although enrollment in nursing programs is on the rise, it still isn’t sufficient to meet growing demands. The American Association of Colleges of Nursing (AACN) points to data that suggests that the country will need more than 200,000 new nurses each year until 2026 to fill new positions or replace retiring nurses. This shortage is especially acute in areas such as education and for certified family nurse practitioners who can provide primary care without a doctor’s direct supervision. In some cases, healthcare providers can resort to hiring travel nurses, who go to different clinics or hospitals to fill temporary shortages. Some nurses move to specialized areas rather than remaining in primary care. There is also an acute need for specialist nurses.[7]
Health Aides: At the low end of the healthcare pay spectrum are residential and nursing home health aides. As the population ages, demand for these workers is outpacing supply.
Healthcare Educators: A need for nurse practitioners means that schools need faculty members who can teach in master’s degree programs and oversee clinical practice for aspiring nurse practitioners. Some nursing schools may even need to restrict enrollment because of a lack of nursing faculty.
Midwives: They are qualified, with a master’s degree and two years of clinical training, to provide proper care during and after childbirth. Furthermore, midwives can provide more personal attention, which could lower the mother and infant mortality rates, which are higher in the U.S. than in other wealthy countries. The U.S. also needs more midwives who can address a shortage of O.B./GYNs and issues such as an abnormally high rate of cesarean sections in the U.S. Currently, midwives only attend about 8% of births in the U.S. The State of the World’s Midwifery 2021 report puts the current worldwide shortage at 900,000—a critical shortfall considering an estimated 4.3 million lives could be saved annually by 2035 were midwife coverage universally available.[7]
Photo by Vladimir Fedotov on Unsplash
Reasons For Shortage of Healthcare Workers
The reasons for the global healthcare staffing shortages are complex and varied. The AAMC reports that by 2032 the over-65 population will grow by 48%. The problem of healthcare worker shortage has become especially acute recently due to this aging population, including the so-called Baby Boomer generation. People in this demographic spectrum often require more medical care, often from physician specialists. Advances in medicine also mean that people are living longer overall, and managing more chronic conditions as they age. Unfortunately, many working physicians will also be reaching retirement age along with the rest of the Baby Boomers. Rural areas could experience more problems because of the physician shortage than urban areas.[8][9]
Salient Reasons(10)
· An Aging Population. As people live longer, they require more medical attention, particularly ongoing services to treat chronic diseases such as heart disease, diabetes, and most forms of cancer. Meanwhile, doctors and nurses are starting to retire faster than they’re being replaced.
· Lack of Instructors. One major factor contributing to the shortage of clinicians is the lack of qualified faculty members to train and educate them, especially at nursing schools.
· Relatively Low Pay for the Rigors of the Profession- Compared with the general population of workers, healthcare practitioners are paid well but the cost, academic rigor, and time commitment of a medical education continue to discourage many from entering medical fields in the first place. For doctors, the fully loaded costs of an undergraduate and medical school education are much higher than the nonmedical professions which require a smaller up-front investment and promise higher pay for less stressful work.
· Clinicians’ typical workdays—marked by long hours, a frenetic pace, emotional duress, deadline pressures, and high-impact decisions—put them at a high risk of burning out. The burden of administrative work, such as having to constantly update electronic health records, is yet another cause of burnout. Burnout (overworked employees are leaving the profession at an accelerating rate) so limited talent pipeline.
. Rise in chronic conditions such as diabetes, heart disease, cancer, and Alzheimer’s disease (leading to overextended staff at hospitals and long-term care facilities)
. Nation’s inability to produce enough doctors and nurses to meet growing demand (partly because of faculty shortages at nursing and medical schools).
. Relatively low compensation levels
. Relatively high job demands
. High education requirements in those fields and the rigors of the medical profession.
Way Forward: Strategies for Filling the Shortages(11)
There’s no magic pill as the reasons and the solutions for the staffing crisis are highly complex. Alleviating the crisis will require a combination of education reforms, government policy initiatives, new healthcare provider operating models, and technology-driven human resources best practices. The healthcare worker shortage isn’t just a provider HR issue. It’s also a public health priority. Numerous studies have shown that improving clinician-to-patient ratios improves patient outcomes and leads to fewer adverse events, complications, and hospital readmissions. One recent study found that each additional patient per nurse is associated with a 12% higher chance of in-hospital mortality.[10][11]
· Adjust Scheduling- To promote a healthier work-life balance, the employers offer their practitioners and support staff flexible schedules, including staggered start times and overlapping shifts, or set at their schedules or work from home part of the time.
· Healthcare Workers Be Given a Voice- By giving employees more of a voice in the organization, healthcare employers create a workplace environment that builds loyalty and engagement—the type of environment that attracts the best and brightest people and encourages them to stay. Conduct regular employee surveys and seek feedback on ways to improve the organization. Connect employees—and, where desired, with professional counselors—for advice and support in developing their careers, coping with stress/mental health status, and dealing with other personal and professional matters.
· Spread Responsibilities Around- Nurse practitioners and physician assistants are already taking on many of the responsibilities that were once the exclusive domain of fully credentialed MDs, such as diagnosing patient conditions and prescribing medications. Healthcare systems are also training and educating caregivers to take on different or more specialized critical care and other responsibilities on short notice. Meanwhile, some of the hands-on care and time-consuming jobs once left to nurses—for example, drawing patients’ blood, giving them IVs, bathing and feeding them, and taking care of certain administrative tasks—can also be delegated to less credentialed workers.
· Customize Recruitment- Finding skilled doctors, nurses, technicians, and other scarce healthcare professionals isn’t as simple as posting job ads. Identifying and attracting people likely to slot well into any organization’s culture requires a customized search conducted by specialized headhunters with the support of the latest recruiting tools.
· Invest in Diversity and Equity- Expanding the pool of doctors, nurses, and other healthcare professionals will require a national effort—starting at the primary and secondary school levels to pursue a course of study and ultimately a career in those fields. Some high school students in economically depressed communities may be offered free training and guaranteed a job interview for entry-level positions. Gender pay gaps if exist in such fields have to be addressed.
· Promote Public Health and Preventative Measures. By giving people, the resources and knowledge to remain healthy, the countries can lower their need for medical services.
· Attract More Nurses to Primary Care Roles. Primary care nurses can help alleviate physician shortages by offering basic care to patients who do not necessarily need a physician’s care. They can help manage chronic conditions and offer self-care advice that can help people manage their conditions and general health so that they require less medical attention in the future.
· Provide Online Healthcare Degrees and Certificates. Online healthcare degrees can make healthcare careers more accessible to more people. Of course, these careers still require clinical training, but students can complete classroom work online.
· Increasing Policy Initiatives Aimed at Supporting Human Resource Development. Policies can make it easier for healthcare human resources professionals to find qualified personnel, offer on-the-job training, and make training more accessible to people who want to enter the healthcare field.
· Collecting Reliable Data for Health Databases. Having access to more data can lead to more streamlined healthcare services. Providers can improve outcome performance and make data-driven decisions about care and treatment if they have access to more information.
· Giving Healthcare Workers a Voice in Shaping Legislation and Policies. Healthcare workers are the most qualified to make decisions about how to change their industry for the better. If they can offer insights to government lawmakers and industry leaders, they may be able to bring about changes that make their jobs easier and make them more effective in clinical settings.
Technological Solutions To Alleviate Nursing Shortages And Physicians
Several technological solutions in healthcare aim to alleviate staffing shortages. Many of these solutions are telemedicine-based:
Telemedicine: Telemedicine allows healthcare providers to consult with patients remotely through video conferencing, phone calls, or other digital communication channels regardless of location (ambulatory or acute). This technology will help reduce the need for in-person consultations or in-person monitoring, freeing healthcare providers to focus on other tasks.
Wearable Technology: Wearable devices such as smartwatches and fitness trackers can monitor patients' vital signs and provide real-time updates to healthcare providers. This technology can help healthcare providers monitor patients remotely and intervene if necessary.
Electronic Health Records (EHRs): EHRs provide a centralized database of patient information that with the proper digital health tools can be accessed by healthcare providers from anywhere. This technology can help reduce the amount of time healthcare providers spend on administrative tasks, allowing them to focus on patient care.
Real-time Clinical Decision Support Systems and Smart Patient Record Viewers and Dashboards: These technologies use AI/ML, autonomous monitoring and alerting of conditions and bundle element delivery, to aid nurses and physicians in effectively using the massive amount of information in the EHRs.
While technological solutions can help alleviate staffing shortages in healthcare, they must be implemented thoughtfully and carefully to ensure they are effective and safe for patients and healthcare providers alike and deliver verifiable ROIs. While these technologies will help alleviate staffing for both the nursing shortage and physician shortage, the selection process should include steps to ensure the technologies that are implemented will make the clinical workflow process easier and more efficient for the clinical staff. Some technologies require significant training to effectively use them. The most effective technologies are designed to be intuitive and easy to use. Some of these technologies may pose risks to patient privacy and data security if not implemented and managed properly. (11)
The physician shortage and nursing shortage are continuing to grow with multiple contributing factors that cannot be solved without the help of innovative technology. Technology and automation play a vital role in helping healthcare systems keep up with the growing demand for technology. The many strengths of the healthcare workforce; provision of basic and advanced specialty care in numerous types of acute care and community-based settings; delivery of public health, school health, and home health services; and compassion in caring for vulnerable populations in rural and underserved locations, as well as the public’s positive perceptions of and trust in nurses, will be tested by a variety of challenges that will develop over next decade. These challenges will widen gaps in the size, distribution, diversity, and expertise of the full spectrum of the nursing workforce, gaps that will need to be addressed to help achieve health equity and reverse the trajectory of poor health status too often found in communities across the nation.
Among these challenges is the growing population of older people, many of whom, particularly frail older adults, have multiple comorbid conditions that increase the complexity and intensity of the nursing care they require. Healthcare staff at all levels will also be challenged to help expand the capacity of the primary care workforce, provide care to rural populations, improve maternal health outcomes, and deliver more health and preventive care in community-based settings. Projected shortages of physicians in both primary care and non–primary care specialties, combined with projections of decreasing numbers of physicians practicing in rural areas, will increase the demand for Registered Nurses (RNs) and Advanced Practice Registered Nurses (APRNs).
The many gaps in the capacity of the current nursing workforce will need to be overcome if the nation is to build a future workforce that can provide the health care it needs. Such a workforce would address social risk factors that negatively affect individual and overall population health and help ensure that all people can attain their highest level of well-being. Currently, there are insufficient numbers of nurses providing enough of the right types of care to the people who need health care the most, particularly in underserved locations. To overcome these deficits, substantial increases in the numbers, types, and distribution of the nursing workforce, as well as improvements in the knowledge and skills needed to address social determinants of health (SDOH), will be needed. These improvements will occur more rapidly, more uniformly, and more successfully if programmatic, policy, and funding opportunities can be leveraged by health systems, government, educators, and payers, as well as stakeholders outside of the healthcare sector.
References
1. Bhatt, V.R., S. Giri and S. Koirala. 2010. “Health Workforce Shortage: A Global Crisis.” Internet Journal of World Health, Society and Politics7(1).
2. World Health Organization (WHO). 2013. Health Systems. http://www.who.int/healthsystems/topics/en/.
3. World Health Organization (WHO). 2006. The World Health Report 2006: Working Together or Health.
4. World Health Organization (WHO). 2007. The Building Blocks of the Health Systems: Aims and Attributes. Geneva: World Health Organization.
5. AHA (American Hospital Association). AHA hospital statistics, 2018 edition. 2018. [June 15, 2020]. https://www.aha.org/statistics/2016-12-27-aha-hospital-statistics-2018-edition .
6. AAMC (Association of American Medical Colleges). New AAMC Report Confirms Growing Physician Shortage. 2020. [January 10, 2021]. https://www.aamc.org/news-insights/press-releases/new-aamc-report-confirms-growing-physician-shortage
7. Buerhaus PI, Skinner LE, Auerbach DI, Staiger DO. Four challenges facing the nursing workforce in the United States. Journal of Nursing Regulation. 2017;8(2):40–46.
8. Green, A. 2007. Health Planning in Developing Countries (3rd ed.). New York, NY: Oxford University Press.
9. Buerhaus P. Nurse practitioners: A solution to America’s primary care crisis. Washington, DC: American Enterprise Institute; 2018.
10. Fried LP, Rowe JW. Health in aging—Past, present, and future. New England Journal of Medicine. 2020;383(14):1293–1296
11. IOM (Institute of Medicine). The future of nursing: Leading change, advancing health. Washington, DC: The National Academies Press; 2011.